
DIEP Flap Breast Reconstruction
There are a variety of surgical techniques for breast reconstruction. Most mastectomy patients are medically appropriate for breast reconstruction, either immediately following breast removal or at a later time. The best candidates, however, are women whose cancer, as far as can be determined, seems to be eliminated by mastectomy. There are legitimate reasons to delay breast reconstruction. Some women may be advised by their surgeon or oncologist to wait until other forms of necessary cancer treatment are completed. Other patients may require more complex breast reconstruction procedures. Women who smoke or who have other health conditions such as obesity or high blood pressure may be advised to postpone surgery. In any case, being informed of your options concerning breast reconstruction can help you prepare for a mastectomy with a more positive outlook on the future.
Breast reconstruction has no known effect on altering the natural history of breast cancer or interfering with other forms of breast cancer treatment such as chemotherapy or radiation.
The DIEP flap is the most advanced form of breast reconstruction available today. It is the preferred technique performed by Dr. Chaiyasate. The DIEP flap technique of breast reconstruction involves the use of lower abdominal skin and fatty tissue with as little as possible amount of the abdominal muscle. This tissue is transferred to the chest wall region in order to reconstruct a breast mound. The blood vessels providing circulation to the tissue are re-connected to the blood vessels on the chest to re-establish flow of blood to the tissue in the new position. This vascular connection usually requires microsurgical techniques. Following the reconstruction of the breast mound, the lower abdominal incisions are closed. This is a modification of TRAM abdominal muscle flap breast reconstruction, but attempts to preserve the “six-pack” muscle function. In some cases, your plastic surgeon may recommend that a breast implant be inserted underneath the flap to give the breast mound additional projection.
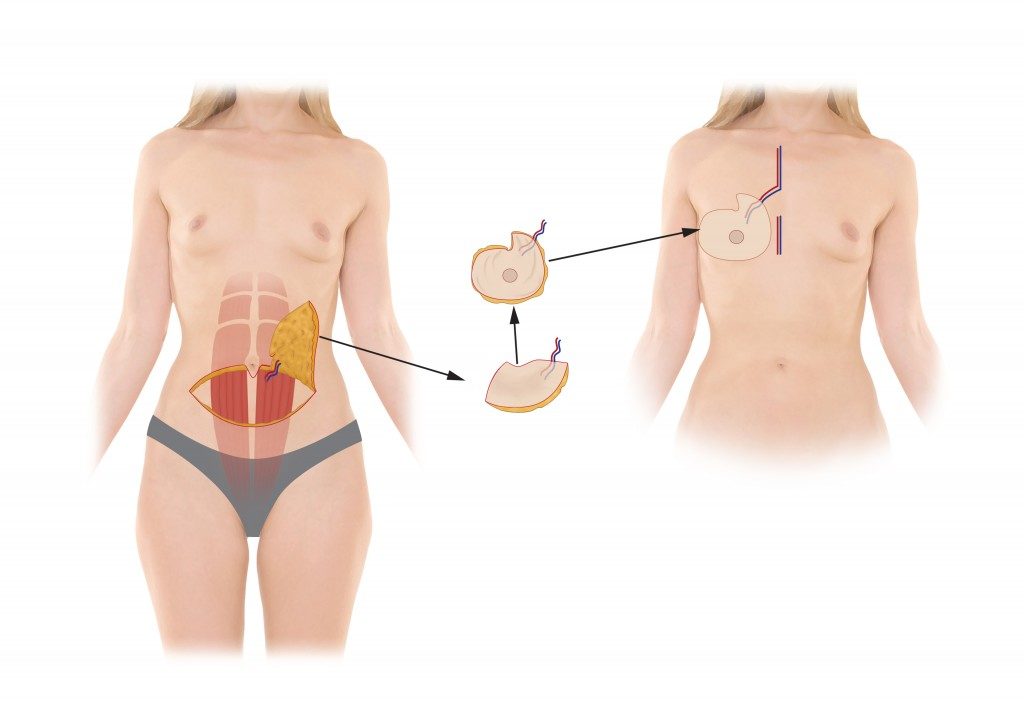
Tissue flap techniques of breast reconstruction are useful in the following situations:
- Inadequate chest wall tissue for breast reconstruction with implants or expanders
- Past history of radiation to chest wall after mastectomy
- Patients with concerns about silicone breast implant/expander
- Failure of earlier breast reconstruction
Contraindications to DIEP flap breast reconstruction procedure exist:
- A patient who is medically or psychologically unsuitable for breast reconstruction
- A past history of abdominal surgery which has impaired DIEP flap blood supply

Stacked DIEP Flap Or Bipedicle-Folded DIEP Flap
For patients seeking reconstruction of one breast, but who do not have much tissue on their lower abdomen or need a larger reconstruction in order to achieve symmetry, using stacked DIEP flaps may be an option. The stacked DIEP flap procedure describes the use of two DIEP flaps to reconstruct a single breast. Similar to DIEP flaps used for double mastectomy reconstruction, the stacked flap procedure utilizes both the right and left halves of tissue on the lower abdomen. The main difference with the stacked flap being that both pieces of tissue are used to reconstruct a single breast.
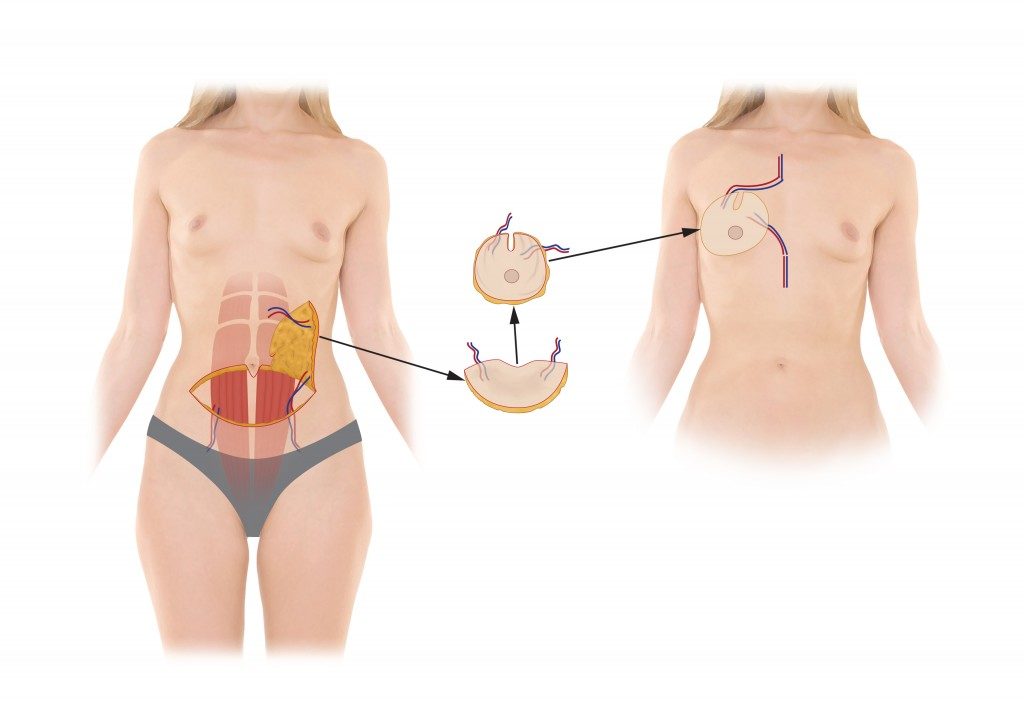
SIEA Flap Breast Reconstruction
The SIEA flap is very similar to the DIEP flap procedure. Both techniques use the lower abdominal skin and fatty tissue to reconstruct a natural, soft breast following mastectomy.
The main difference between the SIEA flap and the DIEP flap is the artery used to supply blood flow to the new breast. The SIEA blood vessels are found in the fatty tissue just below skin whereas the DIEP blood vessels run below and within the abdominal muscle (making the surgery more technically challenging). While the surgical preparation is slightly different, both procedures spare the abdominal muscle and only use the patient’s skin and fat to reconstruct the breast.
Though the SIEA is similar to the DIEP, it is used less frequently since the arteries required are generally too small to sustain the flap in most patients. Less than 20% of patients have the anatomy required to allow this procedure. Unfortunately, there are no reliable pre-operative tests to show which patients have the appropriate anatomy. The decision as to which type of reconstruction to perform is therefore made intra-operatively by Dr. Chaiyasate based on the patient’s anatomy.
For more information about Our Services, or to schedule an appointment, please complete our online form or call us at (947) 274-8300.
